
A baby is considered premature if he or she is born before the 37th week of pregnancy. A full-term pregnancy is 40 weeks, meaning a premature baby did not complete the last few weeks of development in the womb. Premature babies are often much smaller than full-term newborns because the last few weeks of pregnancy are when the baby grows and gains the most weight.
Many different factors can increase the risk of a premature birth. These may include:
- Mother’s health problems, such as high blood pressure or an infection during pregnancy
- Problems with the placenta
- Multiple gestation (twins, triplets or more)
- Previous premature birth
Since prematurity encompasses a birth at any point before 37 weeks, the effects of a premature birth on a baby’s health can vary greatly depending on how early the baby is born. A baby born between 34 and 37 weeks (often referred to as late preterm or near-term) may be larger and have fewer health problems than a baby born before 34 weeks. Babies born before 34 weeks may have a much lower birth weight and underdeveloped organ systems.
Premature babies may have a variety of health problems and may need specialized care in the Riley at IU Health neonatal intensive care unit (NICU). With ongoing advancements in the level of care the NICU is able to provide, babies as young as 22 weeks’ gestation can survive with specialized treatments.
Premature babies may have the following symptoms:
- Inability to maintain a normal body temperature
- Respiratory (breathing) problems
- Cardiovascular (heart and blood vessel) problems—such as patent ductus arteriosus (PDA), a heart condition that causes blood to divert away from the lungs
- Abnormal blood pressure
- Anemia
- Jaundice (yellowing of the skin and whites of the eyes) due to immature liver and gastrointestinal tract
- Kidney problems
- Difficulty feeding because they are not yet able to suck or swallow
- Intraventricular hemorrhage (IVH), which is bleeding in the brain
- Post-hemorrhagic hydrocephalus, which is swelling of the head due to built-up cerebrospinal fluid after an IVH
- Retinopathy of prematurity, a condition in which the blood vessels in the eye do not develop normally and can cause vision problems
Each baby experiences the health problems of prematurity slightly differently. Not every baby will have every symptom.
Treatments
Treatments
The treatments provided after a premature birth will depend on the baby’s specific health problems. Immediately after birth, doctors will start a series of procedures called neonatal resuscitation to stabilize your baby’s condition, address any immediate medical concerns and determine what further treatment is needed. Common treatments for premature babies can include:
- Temperature-controlled beds. A temperature-controlled bed helps your baby retain body heat if he or she has trouble staying warm due to low body fat.
- Intubation and mechanical ventilation. A narrow tube is inserted through the mouth and into the windpipe so that a machine can move air into and out of the lungs. Special types of ventilation may be used for a premature baby’s underdeveloped lungs. These include:
- High frequency jet ventilation. This moves smaller quantities of air through your baby’s lungs at a greater frequency than traditional ventilation.
- High frequency oscillatory ventilation. This moves even smaller quantities of air through your baby’s lungs at a greater frequency, which is helpful when a baby’s lungs are severely underdeveloped.
- Feeding tube insertion. Until your baby can feed normally, a feeding tube may be needed to provide feedings of breast milk or formula.
- IV fluids. An IV may be inserted to put fluids and medicines directly into your baby’s bloodstream to provide hydration or help fight infections.
- Umbilical line placement. This is the insertion of a narrow tube called a catheter into the vein and/or arteries in the umbilical cord area to provide emergency medicines or IV fluids.
- Ultrasound or magnetic resonance imaging (MRI). These imaging tests can help detect whether there is bleeding in the brain, a sign of intraventricular hemorrhage.
- X-rays. These imaging tests can help doctors look at the inside of your baby’s body and identify any internal health problems very quickly.
- Blood tests. Blood testing helps the NICU team keep track of your baby’s overall condition and check for infections. Blood testing is commonly done with a “heel stick,” which means taking a small blood sample from your baby’s foot.
Your baby will receive constant monitoring from the NICU team members to make sure his or her blood pressure, heart rate, breathing rate, body temperature and oxygen levels are normal. If an abnormality is detected, specialized NICU staff and doctors can provide immediate treatment. Depending on the health problems a premature baby has at birth, more specialists may join your baby’s care team at Riley at IU Health:
- If retinopathy of prematurity is detected, a pediatric ophthalmologist will consult with you to decide on the best treatment options. Laser eye therapy is a common procedure that can treat retinopathy of prematurity.
- If your baby has a heart defect, a pediatric cardiologist will evaluate your baby regularly during his or her stay in the NICU and may recommend a surgical procedure to correct the defect.
- If your baby shows neurological symptoms, he or she will be placed on 24-hour continuous electroencephalogram (EEG) monitoring. A pediatric neurologist or EEG technician will monitor your baby and can immediately provide care in the event of a seizure.
- Pediatric surgeons, including neurosurgeons, are on call around the clock in case a baby needs emergency surgery.
Many premature babies may need added specialized care, even when they are ready to leave the NICU. As part of the High-Risk Infant Follow-Up Care Program at Riley at IU Health, a multidisciplinary care team will work with you to form an individualized care plan for your baby’s unique health needs. Along with specialized doctors, this care team also includes physical and occupational therapists and speech-language pathologists who are able to help address day-to-day concerns such as feeding your baby.
Some premature babies may go on to experience developmental delays. The Developmental Pediatrics Department at Riley at IU Health will help coordinate more follow-up care as needed.
What Parents Can Do
A premature birth can be an overwhelming experience for parents, but there are ways you can stay involved in your baby’s care. Ask to see your baby in the NICU and visit him or her often. While you may not pick your baby up until his or her condition is stable, you can still hold hands and touch often.
Once your baby no longer requires major support for organ systems, ask about “kangaroo care” or skin-to-skin care. Having moments of skin-to-skin contact with your baby can help keep him or her warm and provides an opportunity for mom and dad to bond with baby.
You may feed your baby once the doctor says it is safe to do so. NICU team members will help instruct you on the best way to do this, which may involve breast-feeding, bottle-feeding formula or using a breast pump to feed your baby breast milk through a bottle or feeding tube.
You may be ready to return home before your baby is ready to leave the NICU. Remember that your baby is receiving the best possible care, and know that you can continue to visit him or her and touch or hold hands as often as you like. When you return home, you may want to take the time to rest and prepare your home for your baby’s homecoming. This is also a good time to explain the situation to any other children you may have and help them prepare for your new baby’s arrival.
Continuing to visit your baby regularly in the NICU can make it easier to transition to at-home care when your baby is ready to come home with you. If you have family members or friends who would like to visit your baby, check with the NICU staff to find out how many visitors are allowed and whether there are age limits. During cold and flu season, fewer NICU visitors may be allowed in order to protect the babies.
Key Points to Remember
Key Points to Remember
- A baby is considered premature if he or she is born before the 37th week of pregnancy.
- A baby born between 34 and 37 weeks (often referred to as late preterm or near-term) may be larger and have fewer health problems than a baby born before 34 weeks.
- Babies born before 34 weeks may have a much lower birth weight and underdeveloped organ systems.
- Premature babies often require specialized care in the NICU.
- Treatment for prematurity will depend on your baby's specific health problems but always begins with neonatal resuscitation.
Support Services & Resources
Support Services & Resources
Visit the following trusted resources for more information about prematurity.
We offer a broad range of supportive services to make life better for families who choose us for their children's care.
The CDC provides information about fetal development during pregnancy, complications of prematurity and what expectant mothers can do to reduce the chances of having a preterm birth.
This U.S. National Library of Medicine site includes information about the outlook, possible complications and prevention of prematurity.
Learn more about how parents can care for a premature baby in the NICU and at home.
This page from the March of Dimes provides expectant parents with additional education about prematurity.
Prematurity Research
Prematurity Research
Riley at IU Health is a member of multiple research networks that work to improve standards of care for premature babies and advance available treatments. Parents of premature babies can choose to take part in research through the Neonatology Department, which helps to improve care for babies across the state of Indiana and around the world. To read research findings on prematurity, visit the Vermont Oxford Network (VON). VON is a network of hospitals that pool their research findings in the field of neonatology.
Locations
Locations
Locations
In addition to our primary hospital location at the Academic Health Center in Indianapolis, IN, we have convenient locations to better serve our communities throughout the state.
Riley Pediatric Speech Therapy & Audiology
575 Riley Hospital Dr.
Indianapolis, IN 46202
Departments Treating This Condition
Related Stories
Related Stories
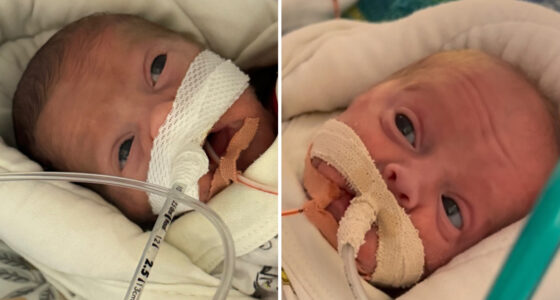
Twin preemies arrive in a snowstorm
A Riley NICU nurse gives birth to twins at just 25 weeks after her husband battles a snowstorm to get her to the hospital.
Continue reading
Afraid to love her, afraid to lose her
Born days after 9/11, Brianna Brooks was so tiny her mother didn’t think she would survive. Now that little girl is about to celebrate her 18th birthday.
Continue reading
